This assessment utilized the latest WHO framework to examine the capacity, performance, and impact of Ethiopia’s Primary Health Care (PHC) system. While historic investments have yielded impressive gains in population health, the assessment highlights critical gaps in quality, readiness, and equitable service delivery.
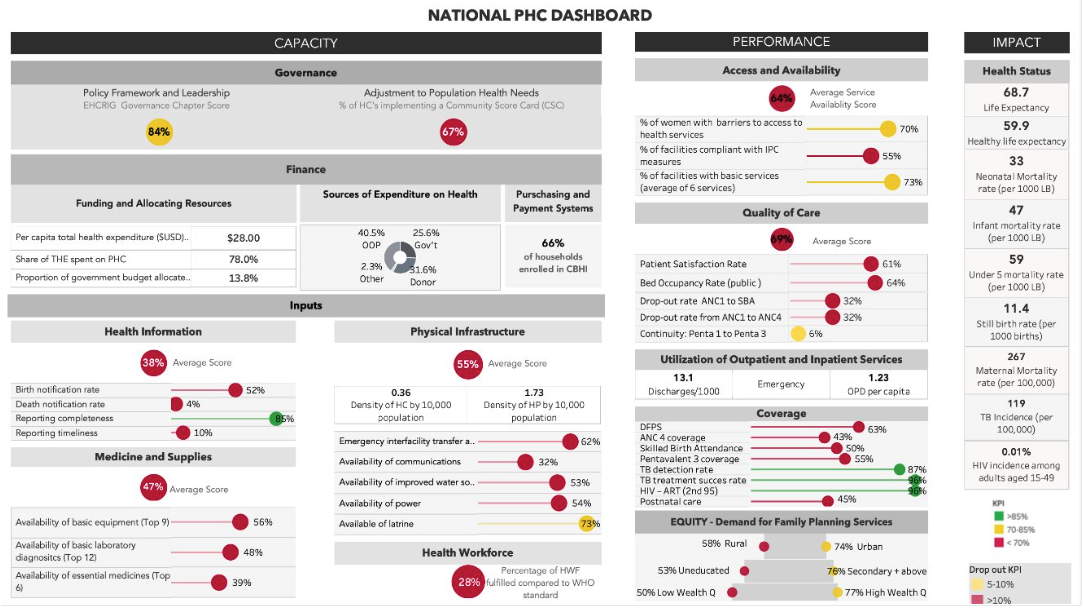
Ethiopia’s health system has a foundational commitment to Primary Health Care (PHC), a strategy that has historically delivered profound health benefits, including a significant increase in life expectancy over the past two decades,. However, a comprehensive assessment conducted in 2023 identified critical operational and systemic challenges that hinder the country’s progress toward achieving Universal Health Coverage (UHC).
The assessment evaluated the PHC system based on three core pillars: capacity (governance, financing, and inputs), performance (access, quality, and equity), and impact.
Key Challenges Facing the PHC System
The PHC structure, designed as the entry point for health services, faces multiple capacity shortages that undermine its ability to provide consistent, high-quality care:
- Low Facility Readiness and Input Shortages: The readiness of health facilities to meet minimum standards for quality care is incredibly low. Nationally, only a fraction of facilities offer all basic client services assessed. There is an inadequate and interrupted supply of essential medicines, medical supplies, and diagnostics,,. Furthermore, many facilities lack basic infrastructure, such as regular electricity and improved water sources.
- Workforce Deficit and Imbalance: The national health workforce density is severely constrained, meeting only about one-quarter of the minimum standard recommended by the WHO for achieving UHC,. This shortage is compounded by an uneven distribution of health professionals, leading to significant regional disparities,.
- Financial Strain on Patients and Facilities: Household Out-of-Pocket (OOP) expenditure remains the largest single source of funding for PHC (40.5%), placing a heavy financial burden on users seeking care,,. Financial barriers are cited as the leading cause of difficulty accessing health care for women,. Moreover, PHC facilities suffer from low or zero reimbursement for providing mandated exempted and fee-waiver services, which jeopardizes the facilities’ ability to sustain equitable, quality service delivery.
Performance Gaps and Equity Divide
Systemic weaknesses translate directly into performance gaps, particularly affecting the quality and equitable distribution of services:
- Suboptimal Quality: The overall quality of care score measured was relatively low,. Adherence by providers to clinical guidelines during diagnosis and treatment is suboptimal, and provider knowledge on diagnostic accuracy needs improvement,.
Equity Gaps: While coverage of key services has improved over the years, progress is not uniform. There is a stark difference in the utilization of key Reproductive, Maternal, Neonatal, and Child Health (RMNCH) services based on a woman's education, wealth, and residence.
Pathway to System Strengthening
To accelerate progress toward UHC, the assessment concludes that the primary focus must shift from expanding infrastructure to comprehensively strengthening foundational system elements, especially financing and institutional capacity,:
- Strengthen Institutional Capacity: Policies and strategies for PHC exist, but institutional capacity must be strengthened at all levels to effectively implement and monitor these strategies,.
- Ensure Adequate and Timely Financing: The government must allocate an adequate budget for PHC activities. A crucial immediate action is establishing an effective mechanism to ensure timely reimbursement to facilities for exempted and fee-waiver services.
- Improve Access and Readiness: Efforts must focus on improving the readiness of facilities by addressing the severe lack of adequate medicines, supplies, and staff training.
Moving forward, the establishment of a dynamic PHC monitoring dashboard will be a critical next step. The dashboard will consolidate key indicators across capacity, performance, and impact—providing real-time, actionable insights to track progress, identify bottlenecks, and guide evidence-based decision-making. By translating assessment findings into a practical monitoring tool, the dashboard will support continuous learning, accountability, and targeted investments to accelerate Ethiopia’s progress toward Universal Health Coverage.
